MEG and Concussions: Advancing the Science of Brain Injury Care
Concussions, often called "invisible injuries," can leave a lasting impact on brain function. Magnetoencephalography (MEG) offers an accurate, non-invasive way to detect, monitor, and treat these injuries by uncovering hidden neural disruptions and guiding personalized recovery strategies.
In case you haven’t read the first three parts of this series, you can check them out here:
MEG: The gold standard for measuring brain function (link)
Comparing MEG to MRI, fMRI, EEG and other brain scanning modalities (link)
Can MEG Help Detect Early Signs of Neurodegenerative Disease? (link)
Curious about your brain function? Book your non-invasive MYndspan analysis or join the waitlist for our future locations today.
Concussions, also known as mild traumatic brain injuries (mTBIs), can disrupt cognitive function, memory, and emotional well-being, yet often go undetected by standard imaging tools. While people often rely on physical symptoms—like dizziness, headaches, or confusion—to identify a concussion, the underlying brain changes are often invisible.
According to recent data from the CDC, over 3.8 million concussions occur annually in the U.S. alone, with a significant rise in cases among youth athletes and aging populations. What’s even more alarming is the long-term impact of repeated concussions, which are linked to conditions like chronic traumatic encephalopathy (CTE) and other neurodegenerative diseases.
Recent trends in neuroscience and technology are reshaping how we diagnose and treat concussions. Unlike traditional methods such as CT or MRI, MEG focuses on the brain’s functional dynamics, offering unique insight into how concussions disrupt neural networks. The further adoption of MEG as a tool to treat concussions could lead to more precise diagnoses, personalized treatment plans, and a deeper understanding of the brain’s recovery process.

The latest MEG literature regarding concussions:
Mild traumatic brain injury impairs neural functioning
https://www.sciencedirect.com/science/article/pii/S2213158221002850
The study reveals that mild traumatic brain injury (mTBI) disrupts neural dynamics, specifically reducing the amplitude and functional connectivity of ‘beta bursts’.
Beta bursts are spontaneous, short-live neural firing patterns seen in typical brain functioning. Here they were impaired in mTBI, showing they could be promising functional biomarker for diagnosing and understanding mTBI.
Repetitive subconcussion results in disrupted neural activity independent of concussion history
https://academic.oup.com/braincomms/advance-article/doi/10.1093/braincomms/fcae348/7815818
This study investigates the neurological impact of repetitive subconcussions, subclinical events that are not quite full concussions - events which are unfortunately common in military and contact sports. The research used magnetoencephalography (MEG) and functional MRI (fMRI) to examine brain function, focusing on Canadian Armed Forces personnel and veterans.
The study showed that neural abnormalities were present in those with more subconcussions than those with fewer events - underscoring the need for preventative measures and monitoring tools, such as MEG, to reduce the risk from cumulative subclinical neurotrauma in military and sports contexts.
Long-term, non-invasive biomarkers that reveal neural ‘slowing’ could enhance our understanding and management of subconcussive injuries.
What role can MEG play in diagnosing, understanding and treating concussions?
MEG technology already plays a significant role in the biological understanding of concussions, particularly in the following ways:
Detection of Brain Abnormalities: MEG can detect subtle functional abnormalities in brain activity that may not be visible through other imaging techniques like CT or standard MRI. MEG can also identify disruptions in neural networks, helping to understand how a concussion has affected brain connectivity and communication.
Assessing Severity and Recovery: By comparing MEG scans taken at different times, clinicians can assess functional abnormalities and monitor brain changes over time. Having an initial scan taken when the brain is in a healthy state establishes a reference point (or baseline) for that person's brain activity under normal conditions. They are particularly beneficial for those at increased risk of head injury, such as athletes, military personnel, and those that participate in high-impact recreational activities.
Return-to-Activity Timelines: Having a baseline MEG scan can help with return-to-activity plans after a person sustains a concussion. A post-incident MEG scan can be compared against the baseline scan. If there’s even a subtle change in brain activity—say, a reduction in communication between areas of the brain involved in memory or motor function— even if the person “feels” fine.
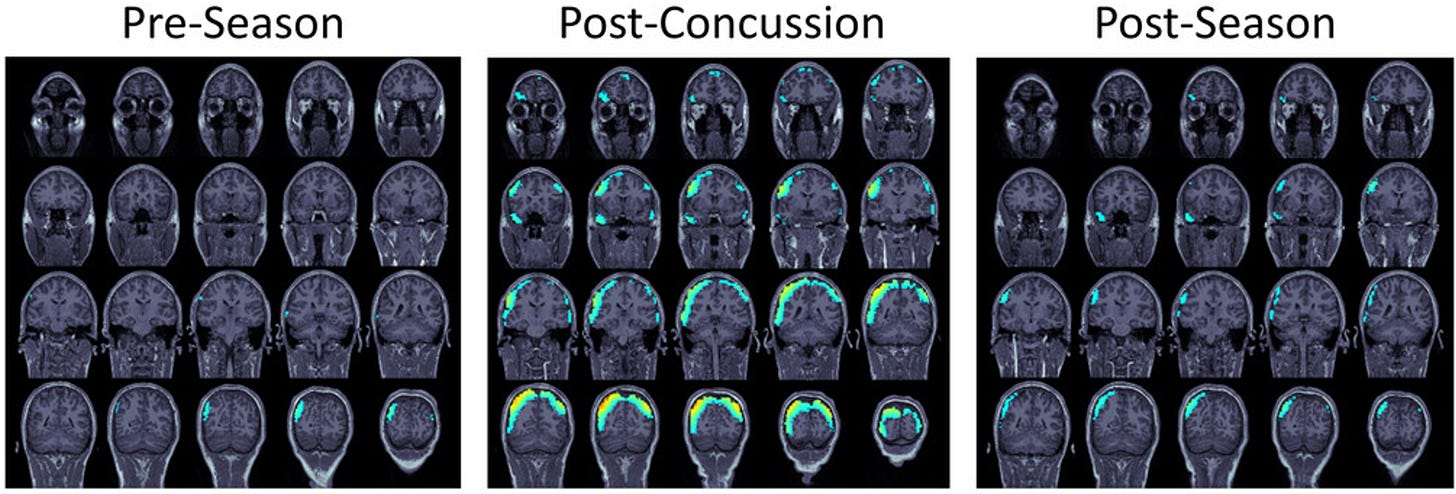
In the example below, MEG scans show delta brainwave activity in different stages of a concussed football player: pre-season (baseline), post-concussion (elevated activity indicating brain disruption), and post-season (partial recovery). Link
Quantitative Analysis: MEG provides quantitative data on brain activity, which can help in objectively tracking improvements , or the persistence of symptoms, which in some cases can persist for months, and even years.
Identifying Specific Affected Areas: MEG can localize specific brain regions that are affected by a concussion, aiding in targeted rehabilitation strategies. It helps correlate symptoms with affected brain areas, such as linking visual disturbances to disruptions in the occipital cortex.
Guiding Treatment Plans: Information from MEG can help tailor rehabilitation programs to address the specific needs of an individual based on which areas of the brain are affected. It can be used to monitor the brain’s response to various treatments, allowing for adjustments in therapy as needed.
Why MEG?
Some of this might be new to you if you haven’t read the other posts in our MEG content series, but several of its advantages also lend themselves well to concussion diagnosis and treatment:
MEG in the future
Our mission at MYndspan is to expand access to MEG technology, and that includes partnerships with leading providers such as Re:Cognition Health. MEG has an important role to play as we progress our understanding of concussions.
MYndspan’s analysis is part of Re:Cognition Health’s concussion pathway:
https://recognitionhealth.com/private-service/brain-injury-concussion/concussion-clinic/
For those who have sustained concussions and are looking for more inputs and information, this pathway includes neurologist input and other diagnostic markers, along with a MYndspan analysis.