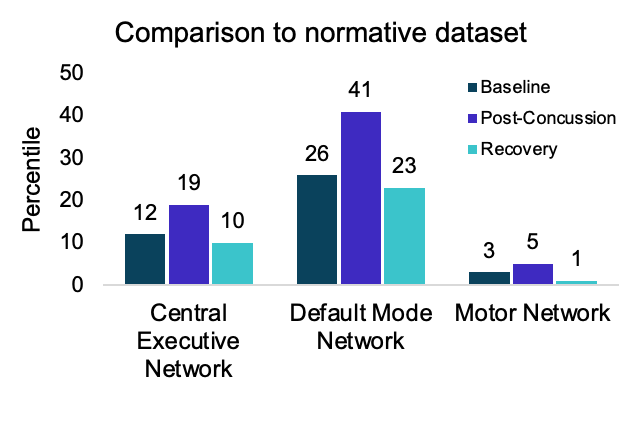Understanding Brain Recovery After Concussion: Crucial Role of Baseline MEG Scans
Case study tracking concussion recovery over time with MYndspan
We’re exploring your interest in a potential crowdfunding campaign planned for early 2025. This would be aimed at our early supporters (like you) as we introduce MEG technology to those looking to better understand and manage their brain health. If you’d like more information, please let us know.
Concussions, often referred to as mild traumatic brain injuries, are much more complex than the term "mild" might suggest. While the visible symptoms of a concussion—headaches, confusion, dizziness, and brain fog—can sometimes resolve within days or weeks, the brain's internal recovery is far more nuanced and can extend over a much longer period. This prolonged recovery involves the restoration of disrupted neural pathways, the rebalancing of brain networks, and the gradual return to normal cognitive and physical function.
Understanding this hidden aspect of recovery is critical for patients, caregivers, and clinicians alike, especially to avoid complications such as returning to activities too soon. A premature return to physical exertion, high-stakes activities, or cognitive demands can increase the risk of further injury, prolonged symptoms, or even permanent damage. This highlights the need for advanced evaluative tools that can go beyond symptom-based assessments and provide clear, measurable insights into brain function. This is where advanced tools like MEG come into play.
In a previous piece, MEG and Concussions: Advancing the Science of Brain Recovery, we explored how MEG technology is transforming the way we evaluate, understand, and treat concussions.
Building on that foundation, this case study dives deeper into a real-world example of how MYndspan’s MEG scans provided valuable insights into the recovery journey of a young adult after a concussion. Through three separate scans conducted over several months, the individual was able to monitor brain progress, identify critical changes, and make informed decisions about recovery timelines.
1. The Baseline Scan: The Brain's Blueprint
Before sustaining an injury, the individual underwent an initial MEG scan to establish a baseline—a detailed "brain fingerprint" unique to their individual brain activity. This scan captured data from critical brain networks, such as:
The Central Executive Network (CEN), which is responsible for focus, working memory, and goal-directed behavior.
The Default Mode Network (DMN), which is active during rest and self-referential thinking.
The Motor Network, which coordinates movement and motor control.
At this stage, CEN activity was measured at the 12th percentile. While this may seem low, it’s important to understand that brain activity varies significantly from person to person, and percentile measurements are only meaningful when compared against the same individual over time. This baseline scan established an essential benchmark for future comparisons, providing clinicians with a personalized reference point.
The value of a baseline scan cannot be overstated. Without it, clinicians are left with generalized comparisons to population averages, which may not accurately reflect an individual’s unique brain function. This data ensures that any changes detected post-injury are specific to the individual, allowing for a more precise understanding of the injury’s impact.
2. Post-Concussion Scan: Detecting Immediate Changes
Roughly six months after the baseline scan, the individual experienced a concussion, prompting a follow-up MEG scan to evaluate the extent of the injury. This scan revealed significant disruptions in brain activity, particularly in areas associated with focus, processing speed, and overall network stability.
The results highlighted three major changes:
DMN Activity: Increased from the 26th percentile to the 41st percentile, reflecting disruptions in the brain’s default network. This increase is consistent with multiple studies (1,2,3), showing that functional connectivity tends to increase after a concussion. This hyper-connectivity may serve as a compensatory mechanism, helping mitigate the effects of concussion on cognition.
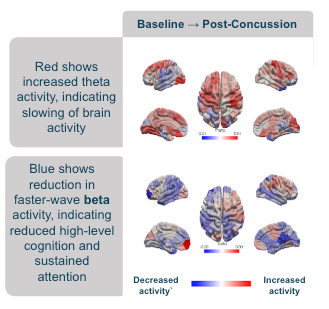
Theta Activity: Showed a noticeable increase. Elevated theta activity is often linked to slower brain processes, which may explain symptoms like brain fog, mental fatigue, and slowed reaction times. Research suggests that higher theta activity can act as an early marker of brain dysfunction after a concussion.
Beta Activity: Decreased significantly, signalling impaired cognitive function, reduced alertness, and difficulty with tasks requiring sustained attention or complex problem-solving. This reduction aligns with findings in the literature, where disruptions in the brain’s balance of excitation and inhibition - reflected in changes to beta waves - help explain the cognitive and motor issues seen after injury.
These findings provided a clear picture of how the concussion altered brain functionality. Importantly, this data highlighted areas of concern that may not have been evident from symptom-based assessments alone.
3. The Recovery Scan: Signs of Healing
Two weeks after the concussion, a third MEG scan was performed to assess brain recovery. Encouraging improvements were noted:
Network Activity: Key functional networks, including the CEN and DMN showed stabilization and returned closer to baseline levels, reflecting improved network function and overall brain recovery.
Theta Activity: Reduced, indicating improved processing speed.
Beta Activity: Gradually returned to baseline levels, supporting better focus and cognitive function. This is consistent with recent research showing increased beta power between visits were linked to a reduction in concussion symptoms, indicating that changes in beta power may reflect clinical recovery, suggesting it can be used useful to track recovery.
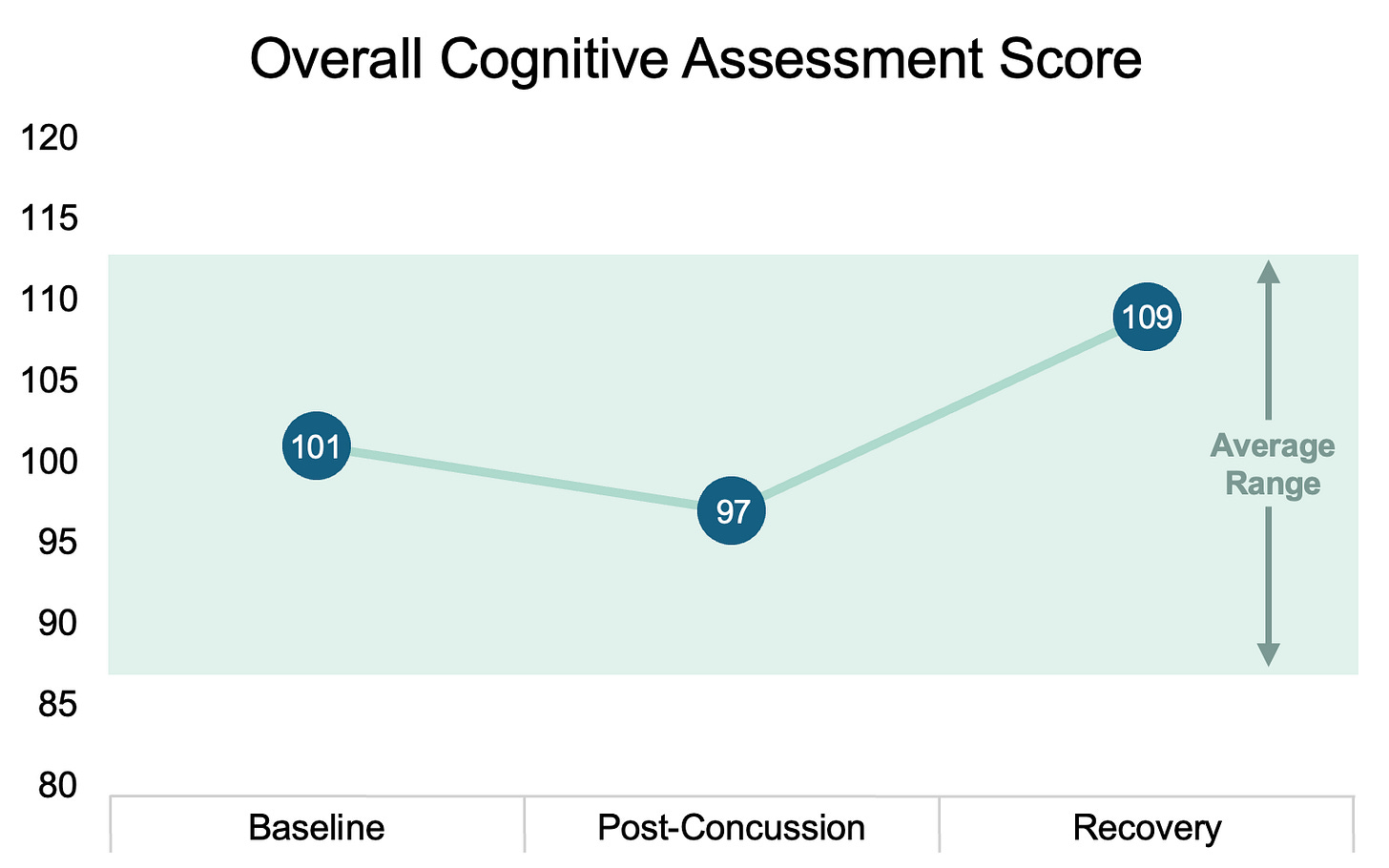
Cognitive Function: Clear cognitive recovery trajectory, with scores surpassing the post-concussion dip by the recovery phase, aligning with brain activity stabilization. This highlights the gradual improvement of cognitive function alongside neurological recovery.
The improvements observed in key brain networks and cognitive assessment scores provided clinicians with confidence that the brain was on its way to full recovery. This data-driven approach allowed for a safe and well-timed return to normal activities.
Why Baseline Scans Matter
One of the most important lessons from this case study is the value of a baseline MEG scan. Without an initial reference point, it would have been challenging to identify the extent of the injury and track meaningful recovery. MEG scans provide objective, quantifiable data, eliminating guesswork and offering a proactive approach to brain health.
Proactive concussion management can significantly improve recovery outcomes. By establishing a baseline before an injury occurs, individuals can ensure that any future changes in brain function are tracked with precision. This allows for more informed decision-making about recovery timelines, activity modifications, and rehabilitation strategies.
Looking Ahead: The Role of MEG in Concussion Care
This case study demonstrates the potential of MEG technology in concussion management. With the ability to monitor brain activity in real-time and compare it against a pre-injury baseline, MEG provides clinicians with the clarity needed to make evidence-based decisions.
For athletes, students, or anyone at risk of concussion, a proactive approach—starting with a baseline scan—could make all the difference in their recovery journey.
If you want to book your baseline scan now or join the waitlist for future locations, visit www.myndspan.com